I received an email earlier this week from a mom who wanted more information about selective dorsal rhizotomy (SDR), and specifically about Dr. Oakes, the neurosurgeon who did it. I’ve mentioned several times that she had SDR when she was three, but because I wasn’t blogging then I haven’t provided a lot of detail.
Since I receive these questions semi-regularly and it’s fresh on my mind, I thought now might be a good time to cover it. I’m using a question-and-answer format because that’s usually how the inquiries come to me. I hope it’s helpful if you’re searching or interesting if you’re curious.
What is selective dorsal rhizotomy (SDR)?
To understand what SDR is you first have to understand what spastic cerebral palsy (CP) is: brain damage that causes nerves to constantly “fire” the message to the muscles to contract, which causes permanent spasticity (and, over time, structural deformities). Spastic diplegia refers to a specific type of CP that primarily or exclusively affects the legs.
In plain language, then, in SDR a neurosurgeon tests sensory nerve rootlets that control the legs to see which ones are “misfiring” and then permanently cuts the most severe of them, permanently disconnecting those wrong signals to the legs. Some spasticity remains, because not all of the wacky nerves can be cut, but the amount varies from person to person.
- For a more detailed explanation, see Wikipedia (and note that SDR has been around since the 1800s, though it wasn’t common until much more recently.)
How old was Sarah Kate when she had it done?
Sarah Kate had SDR one week after her third birthday, in early January 2006. The typical age range for children to have SDR is between ages 2 and 6, though it has been performed on adults. Many factors go into the decision of when to perform SDR, including not just the child’s condition but also his/her personality and level of maturity.
What was she able to do/not do before/after?
Before SDR, Sarah Kate could walk with a walker, but could not take any steps with either canes or independently. An argument could be made that we could have waited to see how much more she could accomplish without it (I know a family whose child had SDR around the same age and they indicated they wish they had waited until she was a little older), but in our case we felt like Sarah Kate had reached a plateau and was unable to make any other significant ambulatory gains. Looking back eight years later, I believe even more firmly that this is true.
We were told before the SDR to expect a one-level improvement in her ambulation (i.e., a child using a walker before should expect to be able to walk with canes after). Sarah Kate went from walker, to two quad canes, to a single cane, to independent ambulation for short distances by the summer of that year. She continued to improve, though at a much slower rate, until she hit her major 10-year-old growth spurt last fall.
- For a video showing Sarah Kate’s progression from before the SDR up until the summer of 2013, visit my YouTube channel.
Where was it done/who did it?
Dr. Oakes at Children’s of Alabama in Birmingham did her SDR.
Why did you go there instead of (fill in the blank)?
Usually this question is phrased as “Did you consider Dr. Park in St. Louis?” and the answer is yes, but only briefly. At the time of Sarah Kate’s surgery, Dr. Oakes had been performing SDR for almost two decades, so we weren’t worried that he lacked experience (at that time, very few doctors had been performing SDR for more than a few years – some still considered it very risky).
The surgeon was just one piece of the puzzle, however. Without focused rehab, SDR is essentially worthless, so it was important to us that the entire team – surgeon, physiatrist, and physical therapist(s) – be knowledgable and experienced about SDR, and we had that at Children’s of Alabama within a short(ish) drive from our house.
What was the recovery like?
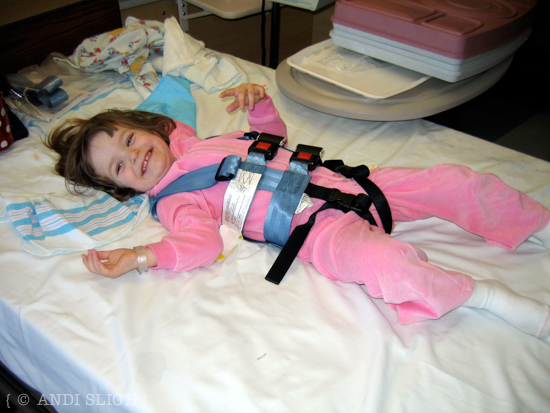
Sarah Kate’s surgery took place on a Wednesday and she initially was sent to pediatric ICU. She would have been out of the ICU after 24 hours but there were no available beds so she had to stay a second night (that was torture for us because we couldn’t stay with her ‘round the clock). She moved to a private room on Friday and was released from the hospital on Saturday.
She had to remain flat on her back until Sunday due to mild concerns that she could leak spinal fluid. I think her experience was atypical and that most children are allowed to sit up a day or two earlier, but I’m not certain. Once she was released from the hospital we were able to manage her pain by stacking OTC Tylenol and OTC Motrin.

How much physical therapy rehab was required? What did they do?
She began intensive physical therapy on the Monday following her surgery and went for four hours per day, five days a week, for three weeks (roughly two hours in the morning and two in the afternoon). Each day began with heat and massage, followed by some typical PT stretching and exercises.
After the first three weeks, she had one PT session each day until May, when she did another three-week session of intensive therapy. The intensive session also included use of the Adeli suit. To help her muscles “be the most they could be” she received Botox injections during the same time period. From May until September, she dropped to two days per week of PT and we supplemented with a pool pass. 🙂 In September, she dropped back to her regular routine of one PT session per week.
- For a blow-by-blow of the experience from beginning to end, visit the blog that I kept for family and friends back in 2006.
How quickly did you see a difference?
We could see a difference in her spasticity on the very first day of rehab. The first thing they had her do after heat and massage that day was to sit “criss-cross applesauce” on the mat. She was unable to sit that way before SDR; her knees would point up toward the ceiling and she would struggle to balance on her tailbone. She opted for a “W-sit” instead with both legs off to one side. The first morning of rehab she could sit criss-cross applesauce, no problem.

Would you do it again?
Absolutely. I’m not certain Sarah Kate would ever have walked independently without it. She almost certainly would never have played softball. She also would likely have had major orthopedic surgery much earlier – probably around age seven – and again at her current age of eleven. Instead, she was able to bypass the first round and we have high hopes for this round, based on Gillette’s assessment that she has very little residual spasticity today.
What has changed with SDR since 2006 when Sarah Kate had it done?
I can’t fully answer this question, but I do know a couple of things: first, it’s more common than it was in 2006. Also, just after Sarah Kate’s procedure, Children’s of Alabama changed the technique used slightly to allow for a much smaller incision (in fact, I believe she was the last child there to have the larger incision). Dr. Park had begun using the smaller-incision-procedure shortly before Dr. Oakes; I assume it has become the standard now. Also, I believe many (most?) surgeons are waiting a little later to perform SDR – age five seems to be most common these days.
Did your insurance cover it?
The SDR, yes. Children’s of Alabama and Dr. Oakes were in-network for us so it was covered like any other surgery, less normal copays and deductibles. Physical therapy was the major expense we faced – she was allowed thirty visits in a calendar year, which only got us to mid-February. We obtained a case manager and were (eventually) granted fifteen additional visits, earmarked specifically for the second three-week intensive program in May. Everything else was 100% out-of-pocket.
That’s the bad news. The good news is that we were able to negotiate some of the costs down, our local therapist set us up on a payment plan, and a group of unknown individuals (to this day, we don’t know who or even how many there were) secretly gifted us $1000 toward her medical bills. It was a rough time, and I worried A LOT, but we always knew we would find a way because she needed it. In the end, it was worth every penny and every hour we spent on the phone with (fill-in-the-blank).


Those photos of baby Sarah Kate are adorable. And the video is awesome!! (I think I’ve seen it before, but it is just awesome– I love how excited she is going up and down the stairs.
I have a hard time looking at the video now – she’s gone downhill so much since those last clips last summer. It was September when the wheels started coming off. Hopefully, though, now that’s she had surgery, she’ll be back where she was (or better!) by the fall.
THANK YOU! You are so sweet to talk to me for so long AND do this blog post. Now I can let my husband and my mom read it:) Thanks for sharing your experience.
Ha! I’m very glad you are happy about it. This post was a last-minute decision, and I paused before I hit “publish” because I hadn’t cleared it with you that I was going to do it. I figured since I didn’t mention any personal details it would be okay. 🙂 I’m glad you found it helpful, and feel free to ask me anything else you want to know.
How’s Sarah Kate doing since the casts came off. Are her heels any better?
They are improving, though not as quickly as I’d like. Crossing my fingers she’s ready to stand on Tuesday!
I can’t view the video on YouTube…it says that it is blocked by Disney Music Company.
Hmmm… What type of device are you using to view it? I just tried with my Mac and it opened fine (albeit with a small ad showing where you can buy the music). Wondering if it’s blocked on mobile pages only?
iPad